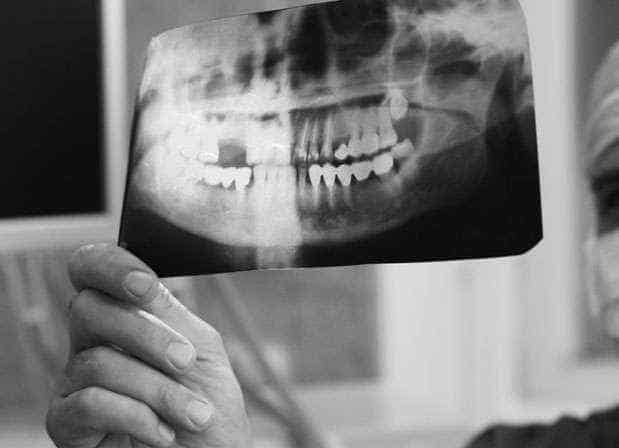
Wisdom teeth or third molars typically erupt between the ages of 17-25. Because there is often a lack of space for them and since they are the last tooth to erupt, wisdom teeth will often rotate or fail to erupt completely, this is known as impaction. Impacted wisdom teeth can cause a number of issues that may necessitate their removal. In this blog we will discuss some of the problems impacted wisdom teeth can pose and when wisdom teeth should be considered for removal.
Pericoronitis: Pericoronitis can be defined as inflammation of the gum surrounding or covering an erupting or impacted tooth. Pericoronitis is a common occurrence for impacted or erupting wisdom teeth and may lead to a bad taste in the mouth, pain, and sometimes infection of the area. Pericoronitis can be temporarily treated with an antibacterial mouth rinse or in more severe cases antibiotics. However, if the tooth does not fully erupt or remains impacted then the inflammation or infection will return. Pericoronitis is one of the most common reasons why wisdom teeth are removed.
Decay and Periodontal disease: Due to their position at the back of the mouth, wisdom teeth can often be challenging to clean and over time this can lead to decay or gum disease. If a patient is having difficulty cleaning a wisdom tooth, the dentist may recommend it be removed even if it is not currently causing problems, this is known as prophylactic removal in that the tooth is being removed to prevent potentially serious complications at a later date. It is important to understand that the decay and periodontal disease may not be limited to the impacted wisdom tooth. A recent article in the British Dental Journal suggested that if a wisdom tooth is partially erupted and impacted in a certain way then it should always be considered for removal, even if it is asymptomatic (1). The authors point to the significant risk of decay of the second molar (the tooth next to the wisdom tooth) which may lead to a deep restoration, root canal, or even loss of this tooth.

Ulceration and Cheek Biting: Cheek biting and ulcerations can occur when an upper wisdom tooth pushes sideways due to lack of space in the jaw. Removal of this tooth will alleviate this ulceration.
Cyst Formation: Inflammatory cysts are sacs of fluid that can form around an impacted wisdom tooth. These cysts can destroy bone, displace the tooth, and may cause damage to adjacent teeth. If a cyst is detected around a wisdom tooth it should be considered for removal.
The Decision to Remove a Wisdom Tooth: As with any medical intervention, both the patient and the treating clinician must weigh up the risks and the benefits of a procedure. The same holds for wisdom tooth removal, after examination including x-rays your dentist will discuss the level of difficulty of removal and any potential risks involved. Among others, this will include the proximity of a lower wisdom tooth to nerves that supply sensation to the lower lip, chin, teeth and tongue. In some cases, there may be risk of injury to these nerves which can lead to a loss of or altered sensation of these areas. Once assessed, the risks for each tooth can be weighed against the advantages of wisdom teeth removal and an informed decision made.
Dr Michael Russo (BCom) (BDent)
- 1. Revolution vs status quo? Non-intervention strategy of asymptomatic third molars causes harm. V. Toedtling, J. M. Yates. July 10, 2015, BRITISH DENTAL JOURNAL, Vol. 219, pp. 11-12.
Warning: Any surgical or invasive procedure carries risk. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.